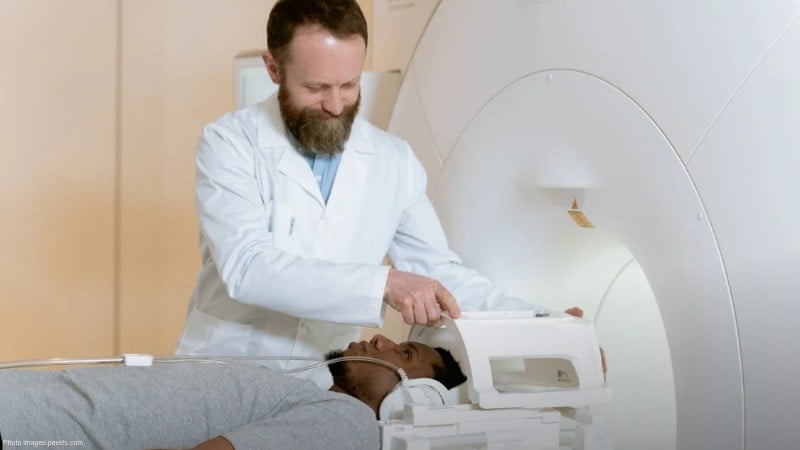
As AI becomes more integral to healthcare, its potential to transform practices is clear, from diagnosing diseases to improving administrative tasks and drug development. However, this potential brings the responsibility to ensure AI is developed ethically, securely, and transparently. In healthcare, where lives are at stake, building trustworthy AI is critical.
This article explores the principles, frameworks, and applications of Trustworthy AI in healthcare, highlighting its role in ensuring patient safety and improving outcomes.
Key Takeaways
The article discusses the principles, frameworks, and practical applications of Trustworthy AI in healthcare, emphasizing the importance of ethical, secure, and transparent AI systems.
- Trustworthy AI in healthcare must follow ethical principles such as human-centered design, transparency, and accountability to ensure patient safety and favorable health outcomes.
- A robust framework for developing Trustworthy AI involves setting clear goals, ensuring high-quality data, extensively testing algorithms, and deploying systems with continuous monitoring and governance.
- Real-world examples, such as IBM Watson in oncology and AI in radiology, underscore the need for stringent ethical oversight to prevent biases and misdiagnoses.
Understanding Trustworthy AI
Trustworthy AI refers to AI systems that operate transparently, safely, and ethically while maintaining high levels of accuracy, security, and reliability.
AI in healthcare has the potential to revolutionize diagnostics, treatment planning, and patient care, but its implementation requires rigorous oversight. Trustworthy AI must avoid biases, ensure patient confidentiality, and meet high standards of safety and performance.
As such, the focus should be on ensuring that these systems are developed according to ethical principles and best practices, with continuous oversight to mitigate any risks.
Key characteristics of Trustworthy AI
AI systems in healthcare must be reliable, providing accurate results in critical areas like diagnosis and treatment. They should also be robust, functioning well in various scenarios, from emergencies to routine screenings. Data integrity is key, ensuring patient information is secure and ethically handled.
Human-centered design is crucial, emphasizing patient-focused decision-making and oversight. Clear accountability mechanisms must be in place, holding healthcare providers and AI developers responsible for errors or failures.
Examples of untrustworthy AI include biased models leading to inaccurate diagnoses and lack of transparency, making it difficult for professionals to understand decision-making processes. Addressing these issues is essential for positive contributions to patient care.
Principles of Trustworthy AI
The foundation of trustworthy AI lies in adhering to specific principles that ensure these systems operate ethically and responsibly. Below are the principles of trustworthy AI, each of which guides organizations in designing, implementing, and governing their AI systems.
1. Humane: AI systems should be designed with the well-being of patients in mind, ensuring that AI contributes positively to their health outcomes. The technology should never replace human oversight but rather complement it by enhancing the quality and efficiency of care.
2. Consensual: Obtaining informed consent from patients for data usage is critical. Patients must be fully informed about how their health data will be used and must grant permission for its use in AI models. Ethical concerns around data privacy must be addressed through clear consent frameworks.
3. Transparent: Transparency in healthcare AI is essential for building trust and enabling scrutiny. For instance, diagnostic algorithms should clarify their reasoning to help healthcare professionals verify results.
4. Accessible: Healthcare providers must have access to the necessary tools and knowledge to assess AI’s decisions and outcomes. This accessibility ensures that they can interpret the AI’s suggestions and make well-informed decisions, preserving human oversight in critical healthcare decisions.
5. Agency-imbuing: Healthcare technology should offer clear, understandable recommendations and allow patients to challenge decisions or provide feedback, ensuring human agency is maintained.
6. Explainable: In healthcare, AI explainability is crucial. Doctors must understand how AI reaches conclusions, especially for diagnoses and treatment recommendations, to effectively communicate with patients about their options.
7. Private and secure: Patient privacy must be prioritized when using AI in healthcare. AI systems should adhere to strict data security protocols, such as encryption and access controls, to protect sensitive health data from unauthorized access and misuse.
8. Fair and quality data: AI models in healthcare rely on diverse, representative, and unbiased data to avoid misdiagnoses and unfair treatment. If trained on data from just one demographic, AI may fail to identify health conditions in other groups.
9. Accountable: Clear accountability structures must be in place to hold healthcare providers, AI developers, and regulators responsible for any issues, including errors, biases, or harm caused by AI in medical settings.
10. Traceable: AI models should have traceability built into their design. This means that healthcare providers should be able to track how decisions are made and identify the underlying causes of errors. Traceability also allows for the auditing of AI systems to ensure compliance with regulations and ethical standards.
11. Feedback-incorporating: AI systems in healthcare should be open to feedback and continuous improvement. Regular evaluations and updates based on real-world use cases help improve AI performance and reduce biases, making the technology more reliable over time.
12. Governed and rectifiable: AI systems must be governed by clear policies and regulations to ensure compliance with healthcare laws and ethical standards. Furthermore, there should be mechanisms to rectify errors when they occur, ensuring that patient safety is never compromised.
Framework for building Trustworthy AI in healthcare
While the principles provide the ethical foundation, a robust framework is necessary for organizations to effectively build, deploy, and maintain trustworthy AI. Below is a four-step framework to guide the creation of AI systems that align with the aforementioned principles.
AI strategy, design, and planning: During the planning phase, healthcare organizations must set clear, patient-centered AI goals aligned with their objectives. Ethical concerns like patient data privacy and the risk of exacerbating health disparities must be addressed. Adequate resources, including time, budget, and expertise, are essential to maintain system integrity.
Data: The success of AI in healthcare relies on high-quality data. Organizations must develop a strong data strategy to ensure accuracy, representativeness, and compliance with privacy regulations like HIPAA. Data collection should be transparent and include measures to prevent biases that could affect patient outcomes.
Algorithm: AI models used in healthcare must be thoroughly tested to ensure their reliability and fairness. This includes using diverse datasets, testing the algorithms in various healthcare scenarios, and continuously evaluating their performance. The AI system should be able to handle unexpected inputs or edge cases while maintaining accuracy.
Deployment and governance: After testing and approval, the AI system enters deployment, requiring ongoing monitoring for performance and safety. Regular audits should assess adherence to ethical standards and patient safety guidelines, with a governance structure in place to address emerging issues in real-time.
Real-world examples of AI in healthcare
AI applications in healthcare have shown great promise, but they also face challenges that highlight the importance of ethical oversight:
IBM Watson for oncology: Watson’s AI was initially praised for its potential to revolutionize cancer care, but its shortcomings in providing accurate recommendations led to setbacks. IBM Watson for Oncology faced issues such as the AI recommending unsafe treatments due to flawed data.
AI in radiology: AI tools for reading medical images, like X-rays and MRIs, are effective in diagnosing conditions like pneumonia and breast cancer. However, concerns about misinterpretation, especially in diverse populations, highlight the need for AI systems to be trained on data from all demographics to prevent biases.
Predictive models in emergency rooms: Some hospitals use AI to predict patients needing emergency interventions, which can be useful. However, there’s an ethical concern about over-reliance on AI, as it could lead to misdiagnoses without human judgment.
Why Trustworthy AI matters in healthcare
Trustworthy AI is vital in healthcare due to its impact on patient safety, treatment outcomes, and efficiency. Addressing ethical concerns like privacy, transparency, and fairness is essential to prevent harm and ensure AI serves patients’ best interests.
Ethics in AI helps reduce risks of misdiagnosis, bias, and unequal access to care, building trust among patients, providers, and developers. AI transparency and accountability are key for healthcare providers to confidently use AI, knowing the systems are safe, ethical, and effective.
As AI grows in healthcare, building trustworthy systems that prioritize patient safety, data privacy, and fairness is essential. By following ethical principles and a clear development framework, healthcare organizations can create AI tools that enhance patient care and build trust. Trustworthy AI will shape a safer, more efficient, and equitable healthcare future.