A recent study by the American Medical Association found that 85% of physicians now use telemedicine in their practice, up from just 25% in 2018. This dramatic shift hit home for me last month when I needed a quick consultation for a persistent cough. Instead of waiting days for an in-person appointment, I hopped on a video call with my doctor within hours. It was convenient, but I couldn’t help wondering about the broader implications of this digital health revolution.
This blog post explores the top 8 advantages and disadvantages of telemedicine in 2025. We’ll dive into improved access to care, enhanced continuity of care, cost savings, increased convenience, improved patient satisfaction, access to specialists, enhanced care coordination, and privacy and security concerns. Each aspect will be thoroughly examined, providing a comprehensive overview of telemedicine’s impact on healthcare delivery.
Key Takeaways
- Telemedicine significantly improves healthcare access, especially for rural patients
- Enhanced continuity of care leads to better management of chronic conditions
- Cost savings benefit both patients and healthcare providers
- Increased convenience boosts patient satisfaction and engagement
- Access to specialists expands treatment options regardless of location
- Improved care coordination reduces medical errors and enhances treatment efficiency
- Privacy and security concerns remain a significant challenge in telemedicine adoption
- Technical reliability and internet connectivity issues can impact telemedicine effectiveness
| Advantage/Disadvantage | Accessibility | Quality of Care | Cost-Effectiveness | User Experience | Data Security | Technical Reliability |
|---|---|---|---|---|---|---|
| Improved Access to Care | 5/5 | 4/5 | 4/5 | 4/5 | 3/5 | 3/5 |
| Enhanced Continuity of Care | 5/5 | 5/5 | 4/5 | 4/5 | 3/5 | 4/5 |
| Cost Savings | 4/5 | 3/5 | 5/5 | 4/5 | 3/5 | 3/5 |
| Increased Convenience | 5/5 | 4/5 | 4/5 | 5/5 | 3/5 | 3/5 |
| Improved Patient Satisfaction | 4/5 | 4/5 | 4/5 | 5/5 | 3/5 | 4/5 |
| Access to Specialists | 5/5 | 5/5 | 4/5 | 4/5 | 3/5 | 4/5 |
| Enhanced Care Coordination | 4/5 | 5/5 | 4/5 | 4/5 | 3/5 | 4/5 |
| Privacy and Security Concerns | 3/5 | 3/5 | 2/5 | 2/5 | 1/5 | 3/5 |
Criteria Breakdown Summary
We’ll evaluate each of the advantages and disadvantages of telemedicine based on six key criteria: accessibility, quality of care, cost-effectiveness, user experience, data security, and technical reliability. This comprehensive approach ensures a balanced assessment of telemedicine’s impact on healthcare delivery in 2025.
Improved Access to Care
Best Known for Bridging Geographical Gaps
Connecting patients with providers, regardless of physical distance, has been a massive game-changer in healthcare. Most of us have either experienced the convenience of telemedicine or know someone who has. I was awestruck when, several years ago, a colleague consulted with her physician via telemedicine while out of state on a work trip. Ninety minutes later she picked up antibiotics at the pharmacy next to her hotel and was on her way to wellness.
This section highlights a few of the features, pros, and cons of telemedicine when it comes to improving access to care.

Source: telemedtrends.com
Features
Telemedicine platforms vary in their features, but they are all designed with efficiency and improved health outcomes in mind. Virtual waiting rooms that sometimes have a call-back feature, AI-powered triage systems that prioritize urgent cases, and the potential to use tech wearables for monitoring of vitals in real-time are just a few ways telemedicine has improved access to care and given providers even more insight into their patients.
Pros
The CDC in the United States says that “healthcare equity exists when everyone has a fair and just opportunity to attain their highest level of health.” Telemedicine has reduced unnecessary travel for patients and enabled faster, more frequent check-ins. This reduces health complications and leads to better overall health outcomes, especially for those with chronic conditions or who are homebound or located in rural locations. It also reduces the out-of-pocket costs of healthcare for patients.
Cons
While telemedicine has numerous benefits, it doesn’t work for everyone or all the time. Internet connectivity is required, and the apps and user interfaces can be confusing for less tech-savvy patients. Not all diagnoses can be made remotely, and some people simply prefer face-to-face interactions with their providers.
Criteria Evaluation
- Accessibility: 5/5 – Significantly expands healthcare reach
- Quality of care: 4/5 – Enables more frequent check-ins but has some limitations
- Cost-effectiveness: 4/5 – Reduces travel expenses and lost work time
- User experience: 4/5 – Convenient but may not suit all preferences
- Data security: 3/5 – Potential risks with digital transmission of health data
- Technical reliability: 3/5 – Depends on internet connectivity and device quality
Community Reviews and Expert Recommendations
Improved access to care is one of telemedicine’s most significant benefits. Jessica Peck, a nursing professor at Baylor University, summarizes it well: “What telehealth is doing is increasing access not just to healthcare, but to quality healthcare.”
Where to Find More Information
For more details on telemedicine’s impact on healthcare access, visit the American Telemedicine Association website: American Telemedicine Association.
Enhanced Continuity of Care
Best Known for Consistent Patient Monitoring
Matt Mullenweg, the founder of WordPress, once said, “Technology is best when it brings people together.” Technology is often at its best in telemedicine, especially regarding continuity of care. It strengthens patient and provider connections, provides consistent vitals monitoring, and allows for timely interventions. On the other hand, ask any provider, and they will tell you there are days they literally want to throw their device out the window, and as patients, many of us can relate. This section will outline some of the advantages and disadvantages of telemedicine when it comes to enhanced continuity of care.
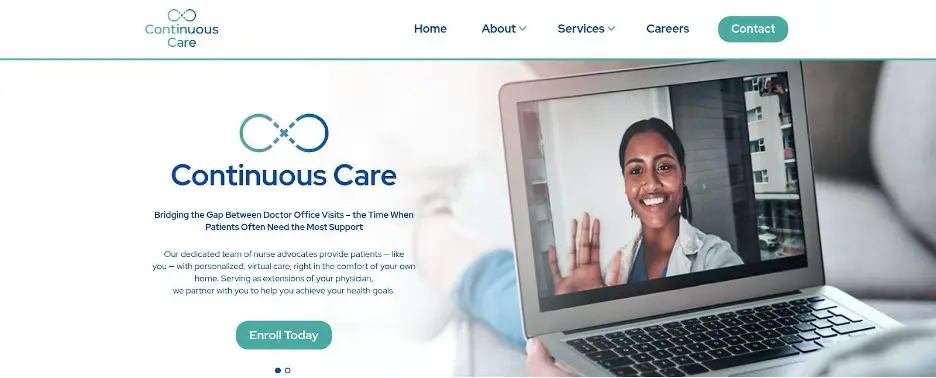
Source: continuouscare.com
Features
Telemedicine platforms have several useful features for patient monitoring. Many now have auto- or self-scheduled virtual check-ins, can monitor vital signs and symptoms remotely, and remind patients to take medications. Integrating electronic health records into one place is brilliant and supports case management efforts among providers.
Pros
Telemedicine creates pathways for improved patient monitoring. It encourages patients to take an active role in their healthcare, allows for real-time adjustments to treatment plans, and can reduce hospital readmissions, resulting in savings of as much as $150,000 per year in savings per nursing home. For patients with chronic conditions telemedicine has supercharged their care.
Cons
I once visited a primary care physician that had patient visits scheduled every 45 minutes. He told me he consistently spent 15 minutes with his patients and 30 minutes charting his notes afterward. Technology had led to an increased workload for him as it does for many providers. It also took away from his time with patients—his favorite part of the job. Telemedicine requires patients to commit time and energy to self-monitoring, and it is easy for a provider to become so reliant on the data supplied by the technology that they don’t stop to think about the person behind it. Opponents of telemedicine argue that subtle changes to a person’s health are not easily detected online.
Criteria Evaluation
- Accessibility: 5/5 – Allows for more frequent provider contact
- Quality of care: 5/5 – Improves ongoing management of health conditions
- Cost-effectiveness: 4/5 – May reduce costly complications through better monitoring
- User experience: 4/5 – Convenient check-ins, but some may feel over-monitored
- Data security: 3/5 – More data transmission means more potential risk points
- Technical reliability: 4/5 – Scheduled check-ins allow for tech preparation
Community Reviews and Expert Recommendations
Healthcare professionals often emphasize the positive impact of enhanced continuity of care on patient outcomes, particularly for those with chronic conditions. Study after study shows it also leads to higher patient satisfaction rates and more cost-effective healthcare, which we will discuss in the next section.
Where to Find More Information
For more insights on telemedicine and continuity of care, check the National Institute of Health’s telemedicine resources: NIH Telemedicine Resources
Cost Savings
Best Known for Reducing Healthcare Expenses
From emergency department visits to cancer appointments, telemedicine has significantly reduced healthcare-related costs for patients and providers. One cost study from 2021 estimates cancer patients saved between $147 and $186 per visit! This section explores telemedicine’s features, pros, and cons regarding reducing healthcare expenses.

Source: telemedtrends.com
Features
Telemedicine has ushered in an era of reduced healthcare expenses for providers and patients. Providers have benefited from lower overhead costs and can see more patients despite leasing less commercial office space. Patients appreciate the time and cost savings associated with getting to appointments, and the adult children or primary caregivers who may have had to miss work in the past to drive a parent or loved one are especially grateful.
Pros
The convenience of telemedicine increases patient utilization because people know it will save time and money. It reduces much of the hassle involved in going to a doctor’s office, and because it is less expensive, patients are more likely to connect regularly with their providers. This leads to better opportunities for early intervention and saves patients and providers money in the long term, which are just a few of the benefits of telehealth.
Cons
One barrier to provider adoption of telemedicine is the initial investment cost in software and hardware, not to mention staff training costs. Providers also run the risk of insurance not covering telemedicine services, which can be a barrier to care and might impact their patients’ experience. Finally, being easily accessible through telemedicine can occasionally lead to patients overutilizing services. In a hospital emergency department, some patients are known as “frequent flyers.” The equivalent of telemedicine is “frequent callers.”
Criteria Evaluation
- Accessibility: 4/5 – Lower costs may improve access for some patients
- Quality of care: 3/5 – Cost focus shouldn’t compromise care quality
- Cost-effectiveness: 5/5 – Direct savings on travel, indirect on lost work time
- User experience: 4/5 – Financial benefits improve overall experience
- Data security: 3/5 – Cost-cutting shouldn’t impact data protection measures
- Technical reliability: 3/5 – Lower-cost solutions may have more technical issues
Community Reviews and Expert Recommendations
The potential for significant cost savings through telemedicine is well documented, especially for reducing unnecessary emergency room visits and hospitalizations.
Where to Find More Information
For more details on the economic impact of telemedicine, explore the Center for Connected Health Policy website: Center for Connected Health Policy
Increased Convenience
Best Known for Home-Based Healthcare
Homebound patients and their caregivers are perhaps the biggest beneficiaries of telemedicine. It has revolutionized healthcare delivery by bringing medical consultation and care directly into their homes. Nonetheless, like any form of healthcare, it is not perfect. This section will explore the features, pros, and cons of home-based healthcare delivered through telemedicine.

Source: telemedtrends.com
Features
Today, home-based healthcare includes on-demand consultations, unprecedented scheduling flexibility, virtual waiting rooms, and integration with a patient’s medical devices and equipment, which collects and sends data to providers.
Pros
Going to the doctor’s office can be a chore for the most able-bodied among us; it can be a monumental task for homebound patients and their care providers. Telemedicine eliminates travel time and associated costs and keeps patients out of waiting rooms and healthcare settings notorious for transmitting illnesses. For unpaid caregivers (family and friends), telemedicine has helped chip away at the greater than $600 billion annual cost of caregiving. It also expands one’s provider network beyond their geographical area, allowing access to specialists—a noteworthy benefit of telehealth.
Cons
Despite the significant benefits of telemedicine, it still relies on a stable internet connection and capable devices. If there is a power or internet outage and care can’t wait, patients and caregivers will need to quickly adjust and come up with a backup plan, which could include seeing an unknown provider. Some patients, particularly elderly patients, might miss connecting with their providers in person.
Criteria Evaluation
- Accessibility: 5/5 – Home-based care is highly accessible
- Quality of care: 4/5 – Convenience may lead to more regular check-ups
- Cost-effectiveness: 4/5 – Saves time and travel expenses
- User experience: 5/5 – Major improvement in patient experience
- Data security: 3/5 – Home environments may be less secure than clinics
- Technical reliability: 3/5 – Depends on the patient’s home tech setup
Community Reviews and Expert Recommendations
In 2021, Niteesh Choudhry, MD and Professor of Medicine at Harvard Medical School, said, “The concept of patient-centered care has been in the lexicon for a decade, but medicine is still not really patient-centric. I think a lot of things should be in the patients’ control, and we should help support them in that.” Telemedicine offers patients this support through increased convenience and allows them the opportunity to fully participate in their healthcare. This leads to better engagement, greater care plan compliance, and better patient outcomes.
Where to Find More Information
For more insights on telemedicine convenience, visit the American Medical Association’s telemedicine page: AMA Telemedicine Resources.
Improved Patient Satisfaction
Best Known for Enhancing Healthcare Experiences
While somewhat paradoxical, some telemedicine providers feel more connected to their patients than when they meet them for in-person office visits. The author and philosopher Alexandra Stoddard said, “The home is the center of your soul; it’s a total reflection of your inner life.” Providers often get a glimpse into the home life of their patients during telemedicine visits, and patients sometimes complete a call feeling like their provider has been to their house. Whatever the reason, studies about telemedicine reveal high patient satisfaction thanks to personalized and responsive care.

Source: telemedtrends.com
Features
Telemedicine consistently offers shorter wait times and more frequent provider interactions than in-person visits would allow, as well as easy access to health records, test results, and prior visits. Care plans are easily personalized and tracked over time. This section will explore the pros and cons of telehealth.
Pros
Happy patients involved in their own care are significantly more likely to follow their treatment plan. Telemedicine improves communication between patients and providers through more frequent but often shorter visits. Both lead to better overall health outcomes.
Cons
Despite its benefits, telemedicine may not be appropriate for all patients. For example, older adults with cognition impairment or hearing difficulties may struggle to communicate in virtual settings. Other patients simply prefer face-to-face interactions over video calls, and those preferences should be supported when possible. Another potential challenge to telemedicine is unrealistic expectations for healthcare providers to diagnose remotely. If an in-person visit is recommended following a virtual one, they may frustrate the patient.
Criteria Evaluation
- Accessibility: 4/5 – Satisfied patients are more likely to seek care when needed
- Quality of care: 4/5 – Satisfaction often correlates with better health outcomes
- Cost-effectiveness: 4/5 – Satisfied patients may require fewer resources long-term
- User experience: 5/5 – Direct measure of positive user experience
- Data security: 3/5 – Patients may be less vigilant if overly comfortable
- Technical reliability: 4/5 – Satisfaction suggests reliable tech experiences
Community Reviews and Expert Recommendations
Healthcare studies have shown telemedicine has improved patient satisfaction scores across the board, but that still doesn’t mean it is right for everyone in every situation. Perhaps a hybrid approach would be best for specific diagnoses, or maybe you aren’t comfortable with the technology required to use telemedicine effectively. Ask yourself or your loved one what will provide the best chance for positive outcomes and use that method.
Where to Find More Information
For studies on patient satisfaction in telemedicine, check the Journal of Medical Internet Research: Journal of Medical Internet Research.
Access to Specialists
Best Known for Expert Care Anywhere
Our friends were looking for a pediatric and adolescent gynecologist for their daughter. They finally found one of the two in the state. She was four hours away. Fifteen years ago, they might have needed to plan an overnight trip and pay for an overnight hotel stay. Instead, they made an appointment for three weeks later and saw the provider from the comfort of their own home. Their daughter didn’t even need to miss one minute of school. One of the many pros of telemedicine is access to specialists regardless of geographical location. In this section, we will discuss some pros and cons of accessing specialists through telemedicine.

Source: telemedtrends.com
Features
Virtual consultations with specialists have significantly eased geographical barriers. Telemedicine offers many features, including the option for second opinions, collaboration with care teams that may be in different cities or even states, and access to experts in rare disease treatment and management.
Pros
More than 1 in 4 adults suffer from multiple chronic conditions in the U.S. If you or a loved one are in that number, you know how important it is to have a variety of treatment options without delay. Telemedicine allows for collaborative diagnosis and treatment planning, improving outcomes for complex or rare conditions.
Cons
While telemedicine provides convenience and access to patients, there are cases when it can’t fulfill the need for an in-person specialist examination. Patients can sometimes obtain scans and tests at third-party locations, but the equipment or technicians at those locations may not be suitable for the nuances of complex medical needs. Regulatory, legal, or reimbursement aspects of health insurance coverage may become a barrier, and communication can falter.
Criteria Evaluation
- Accessibility: 5/5 – Dramatically improves access to specialized care
- Quality of care: 5/5 – Allows for expert consultations previously unavailable
- Cost-effectiveness: 4/5 – May reduce travel costs for specialist visits
- User experience: 4/5 – Improved outcomes, but may feel less personal
- Data security: 3/5 – Specialist consultations may involve sensitive data transfer
- Technical reliability: 4/5 – Specialist systems likely to be high-quality
Community Reviews and Expert Recommendations
If you are considering going to a specialist, ask if they have collaborated with patients in a similar situation or how they typically manage geographical distance and telemedicine in patient care. Telemedicine has revolutionized specialized care, but asking questions upfront will help you and your loved one know what to expect if you start down this path.
Where to Find More Information
For more insights on telemedicine and specialist access, explore the Telemedicine and e-Health journal: Telemedicine and e-Health Journal.
Enhanced Care Coordination
Best Known for Streamlined Healthcare Communication
If you or a family member recently had surgery, you might have received bills from multiple parties, such as the hospital or surgery center, the anesthesiologist, and the surgeon’s office. Unfortunately, this is not uncommon—many healthcare systems are fragmented, which can be confusing for patients and providers. Care coordination can help organize patient activities, procedures, and results all in one place. Telemedicine facilitates improved communication among healthcare providers and patients, which leads to better outcomes.
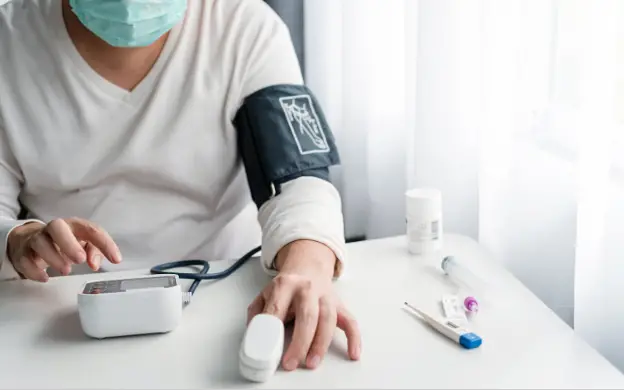
Source: telemedtrends.com
Features
Some telemedicine features include shared electronic health records (EHRs or electronic medical records [EMRs]), integrated care platforms, real-time communication tools, and automated workflows for care coordination, such as medication refill reminders or notifications sent to providers depending on a vitals screening.
Pros
Two telemedicine advantages in care coordination are reduced medical errors and seamless transitions between healthcare providers. When medical staff have accurate, real-time information about their patients, they can see the big picture, which helps them treat their patients holistically and efficiently.
Cons
Care coordination across healthcare systems is not without challenges. Software programs don’t always talk with each other. When they do, providers can be overwhelmed by the information available, especially for complex or older patients. Privacy is also a concern with telemedicine. As the amount of shareable data increases, so does the risk of security or privacy breaches.
Criteria Evaluation
- Accessibility: 4/5 – Improves access to comprehensive care
- Quality of care: 5/5 – Better coordination typically leads to better outcomes
- Cost-effectiveness: 4/5 – May reduce duplicate tests and treatments
- User experience: 4/5 – Less burden on patients to manage their care
- Data security: 3/5 – More data sharing increases potential vulnerabilities
- Technical reliability: 4/5 – Coordinated systems likely to be well-maintained
Community Reviews and Expert Recommendations
Telemedicine is enhancing care coordination and resulting in better overall care for patients, including those seeking care in person or online. Rosemary Ryan, Medicine Director of Clinical Services at the University of Alabama Birmingham, says, “We are expanding the capacity of some clinics that had otherwise been limited by physical space. Meanwhile, the patients who need in-person care are getting it more efficiently.”
Where to Find More Information
For more on telemedicine and care coordination, visit the Healthcare Information and Management Systems Society website: HIMSS.
Privacy and Security Concerns
Best Known for Data Protection Challenges
Our healthcare information and data are very personal. Communicating through technology or sharing data in a digital format can make even the most tech-friendly among us a little nervous. The adoption of telemedicine raises questions about digital security and protecting patient data, one of the potential disadvantages of telemedicine. This section will review the features, pros, and cons of privacy and security in telemedicine.

Source: telemedtrends.com
Features
Modern telemedicine has several features to keep us and our loved ones safe. Multifactor authentication for access, secure video conferencing, encrypted data protocols, and regular security updates and audits play a role.
Pros
Security standards have improved as telemedicine has been increasingly adopted and used in healthcare. Patients and consumers are more vigilant about digital security and trust it more than they did in earlier years, and competition among technology providers has led to innovation and better experiences for those who use it.
Cons
Privacy and security concerns are still a deterrent for many people to use telemedicine, and there have been numerous data breaches among healthcare systems already this year. Data breaches and continually evolving regulations are two of the larger cost-drivers for telemedicine.
Criteria Evaluation
- Accessibility: 3/5 – Concerns may deter some from using telemedicine
- Quality of care: 3/5 – Privacy worries may limit patient openness
- Cost-effectiveness: 2/5 – Security measures can be expensive to implement
- User experience: 2/5 – Privacy concerns can negatively impact experience
- Data security: 1/5 – Direct measure of this critical issue
- Technical reliability: 3/5 – Security measures may impact system performance
Community Reviews and Expert Recommendations
Patients, providers, healthcare systems, and anyone who uses or employs telemedicine should remain vigilant about privacy and security. In 2022, Senator Patty Murray said in a hearing for health and education, “We need to address cybersecurity attacks and ensure they are treated like the national security threat they are because cyber-attacks are on the rise.” Privacy and safety in telemedicine are critical to its continued use.
Where to Find More Information
For guidelines on telemedicine security, check the Health Insurance Portability and Accountability Act (HIPAA) guidelines: HIPAA Guidelines.
Notable Mentions
Potential Technical Issues
Technical glitches can significantly impact telemedicine experiences. From poor internet connections to device malfunctions, these issues can disrupt care delivery and lead to poor patient experiences.
For more on addressing technical challenges in telemedicine, visit: HealthIT.gov Telemedicine Resources
Limited Access for Some Patients
Despite its benefits, telemedicine may not be accessible to all patients due to limited digital literacy or lack of internet access.
Explore initiatives addressing this issue at: FCC’s Connecting Americans to Health Care.
Time Zone Differences
For telemedicine services spanning different time zones, scheduling and availability can become complex, potentially affecting care continuity.
Learn about managing global telemedicine at: WHO Telemedicine Opportunities and Developments.
Language Barriers
Telemedicine can exacerbate communication challenges when patients and providers speak different languages, necessitating effective interpretation services.
Discover solutions at: Language Access in Telemedicine.
Artificial Intelligence
AI is revolutionizing patient care in many ways, including through its capabilities in telemedicine. AI will also have future applications in healthcare. Learn more about AI in healthcare and its real-world applications in telemedicine: How AI is Revolutionizing Patient Care
Frequently Asked Questions
How secure is my health information during a telemedicine consultation?
Telemedicine platforms use advanced encryption and security protocols to protect your data. However, using secure internet connections and following best practices for online safety is crucial.
Can telemedicine completely replace in-person doctor visits?
While telemedicine is highly effective for many health issues, some conditions still require physical examinations. Telemedicine should be viewed as a complement to traditional healthcare rather than a complete replacement.
What equipment do I need for a telemedicine appointment?
Typically, you’ll need a device with internet access and a camera (smartphone, tablet, or computer). Some consultations may require additional equipment, such as a blood pressure monitor or thermometer.
How does insurance coverage work for telemedicine services?
Insurance coverage for telemedicine varies by provider and location. Many insurers now cover telemedicine services similarly to in-person visits, but it’s best to check with your insurance provider for specifics.
What types of medical issues are best suited for telemedicine?
Telemedicine is particularly effective for follow-up appointments, managing chronic conditions, mental health consultations, and addressing minor acute conditions. However, emergencies or conditions requiring physical examinations are better suited for in-person care.
Final Thoughts
Telemedicine has revolutionized healthcare delivery and offers numerous benefits, but it also presents unique challenges. As we navigate this digital health landscape, it’s crucial to weigh the advantages against the potential drawbacks.
Improved access and convenience through telemedicine, regardless of where a patient lives, has forever changed healthcare. Patients and their loved ones are experiencing enhanced care coordination and higher quality care, resulting in better overall health outcomes. Still looking for another advantage of telemedicine? This is all being done while saving money for providers and their patients, a true win-win.
Software reliability and regular internet access are ongoing challenges for some patients. Privacy and security concerns need to be addressed, and patients who are tech-averse or cannot use devices independently may struggle to fully adopt telemedicine.
TeleMedTrends plays a vital role in keeping you informed about these evolving telemedicine dynamics. By staying up to date with the latest trends and insights, you can make informed decisions about your healthcare options in this digital age.
Ready to dive deeper into the world of telemedicine? Visit TeleMedTrends for the latest updates, expert analyses, and comprehensive guides to navigate your digital health journey. Be sure to check out our future outlook on telemedicine trends: Virtual Healthcare in 2025